COVID-19 and Nanotechnology - Nanografi Blog
Coronavirus (2019-nCoV) continues to halt a big part of operations in the world. From manufacture to service sector a lot of domains in public health and economy have been affected. There are test, vaccine, and treatment researches all around world while time is ticking. However, answer might be in nanotechnology to find COVID-19 test, or to develop a vaccine for coronavirus. Below, we discussed the possible nanotechnological contribution to halt novel Coronavirus.
Click Image to Reach Our Other Articles About COVID-19
As a consequence of the global outbreak of the new coronavirus, known as the 2019 novel Coronavirus (2019-nCoV), the World Health Organization (WHO) declared the coronavirus disease 2019 (COVID-19) a pandemic and a state of emergency on January 30 2020. The COVID-19 has been demonstrated to originate in Wuhan City, China. WHO and the Centers for Diseases Control and Prevention (CDC) have officially confirmed human-to-human transmission of coronavirus based on the experiments carried out on three different cases from around the world namely in the United State, Germany and Vietnam. However, WHO had rejected any clear evidence of person-to-person transmission on their Twitter account earlier on January 14th, 2020 referring to a report by the Chinese authorities (https://twitter.com/WHO/status/1217043229427761152) which has to be discussed and scrutinized as well. To this date, coronavirus has infected over one million people from around the world and has claimed more than 55 thousand lives. In most countries, the state of curfew and obligatory quarantine has officially been declared in the hope for suppressing the very fast spread the virus.

Structure and Molecular Biology of Coronavirus
Generally, coronaviruses are a diverse family of enveloped positive-stranded RNA viruses comprising 26 to 32 kilobase genome which is the largest known among all RNA viruses. They are found among an extensive range of hosts capable of infecting species like mammalians and birds and as well as serious health disorders such as gastrointestinal, respiratory, hepatic and central nervous system diseases. Coronaviruses can be classified into four types known as Alphacoronavirus, Betacoronavirus, Gammacoronavirus and Deltacoronavirus among which Alpha- and Betacoronavirus are infectious for mammals; gamma- can infect birds (avian species) and delta- in both avian and mammalians1. The new zoonotic human coronavirus was first reported on January 9, 2020 by the Chinese Center for Disease Control and Protection (CCDC) 2. The betacoronaviruses comprise MERS-CoV, SARS-CoV, mouse hepatitis coronavirus (MHV), bat coronavirus HKU4, bovine coronavirus (BCoV), and human coronavirus OC43. The genome of coronaviruses is encapsulated inside a helical protein shell known as capsid and a lipid molecule. Particularly, the envelope of a virus contain three structural proteins in which the virus assembly involves the membrane protein, nucleocapsid protein and the envelope protein with the spike protein (S) serving as a mediator to ease the entry of the virus into host cells.
Click Image to Find Out More About Nanomaterials in Medicine
In coronaviruses, the spike protein forms crown-like (Corona in Latin) structures coming out of the virus surface used to penetrate the host cells 1. The spike protein itself comprises S1 and S2 where the S1 binds to host cell receptor and S2 for membrane fusion. In fact, the spike protein is the most common target to be neutralized by antibodies and any possible vaccine. The nucleocapsid protein is considered as the most abundant protein in coronavirus and a highly immunogenic phosphoprotein. It should be noted that the nucleocapsid protein hardly ever does mutate and is used as a marker in diagnostic assays.
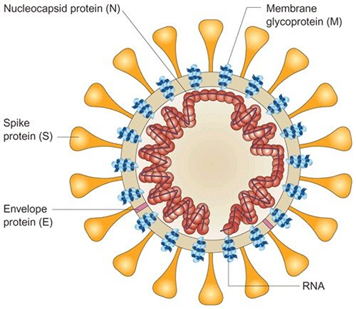
Figure 1. Schematic Diagram of Coronavirus 3
Coronavirus Diagnostics
The respiratory coronavirus disease 2019 (COVID-19) laboratory test involves using the real-time reverse transcription polymerase chain reaction (rRT-PCR) that is carried out on samples collected from the respiratory system by a variety of methods such as nasopharyngeal swab. The test results are revealed a few hours up to two days. The newly developed PCR test in Berlin January 2020 makes the basis of over 250,000 diagnostic kits that has been distributed by WHO. On January 28 2020, a South Korean company designed a PCR-based SARS-CoV-2 detection kit called PowerChek Coronavirus functioning though recognizing the “E” gene within the betacoronavirus’s helical pack. In addition to these, BGI Group (approved by the National Medical Product Administration of China) and Centers for Diseases Control and Prevention of the United States have developed their PCR-based COVID-19 and SARS-CoV-2 diagnostic kits. Based on the PCR method, the RNA of the coronavirus is converted to DNA and the consecutive replication of that as many as millions of times until adequate copies of the replicated DNAs are detectable by an analytical machine called the Quantitative PCR instrument. In the case of recognizing the genetic code of the virus, an individual tests positive for the virus.
Most of the available and newly designed kits are equipped with three assays with each assay being capable of targeting and detecting a different gene in the coronavirus. This means if there are probable mutations, the kits are able to detect and recognize the newly formed generation. In the case of positive responses by one or two assays, the results have to be recorded as the virus genome directory to intercept a new virus outbreak. The available kits can detect target proteins known to be human RNA polymerase protein (ORF1 gene), the nucleocapsid protein (N-gene) and the envelope protein (E-gene). There are also some kits with ability to target the spike protein (S-gene) on the surface of the coronavirus. In addition to the kits now, there are diagnostic platforms as nanosensors likely to replace thermal screening guns used to screen and measure high fever in people who are suspected to have been infected at the airports and borders.
Possible Contribution of Nanotechnology to COVID-19
So far, no evident treatment or vaccine has been suggested for the treatment of COVID-19 except for some conventionally used medication used to improve the immune system against malaria called Chloroquine. However, the interesting and surprising properties of chemical compounds, especially nanodrugs can significantly contribute not only to the medicine and pharmaceutics, but they can also emerge is promising solutions to stop the deadly COVID-19 outbreak across the world.
There is a hope that nanoparticles can make a change sue to their size and intensified properties induced by the severe increase in surface area to volume ratio. The coronavirus structure reveals similarities with nanoparticles. The idea is nanoscale particles, as small as the virus, can interact with spike proteins or bind to them with the consequent disruption of the viral structure through applying electromagnetic radiation mainly infrared light. The resulting structural destruction can suppress the ability of the virus and its genome to multiply and reproduce within a host.
Theranostics, is a newly-emerged are which involves detecting and neutralizing viruses using nanodrugs and nanomedicine with a focus on diagnostics and therapy. Accordingly, there are reports concerning the application of nanoparticles to fight microbes that cause influenza and tuberculosis. Nanoparticles have the ability to intercept the pathogens and viruses due to the possible surface modification and functionalization with a huge amount of reports in the literature. It is possible to modify or functionalize nanoparticles so that they can dissolve the lipid membrane of the viruses or even bind to the spike proteins at S1 and/or penetrate into the envelope and encapsulate the nucleocapsid and RNA. Nanoparticles can be modified/functionalized to attack a particular or a rage of viruses, bacteria and other pathogens. Considering their size, modified nanoparticles can move through the body in bloodstream without causing problems or disrupting other functions, especially those that engage in human immune system and can remain much longer in the body to detect viruses.
References
1. Li, F. Structure, Function, and Evolution of Coronavirus Spike Proteins. Annu. Rev. Virol. 3, 237–261 (2016).
2. Nguyen, T., Duong Bang, D. & Wolff, A. 2019 Novel Coronavirus Disease (COVID-19): Paving the Road for Rapid Detection and Point-of-Care Diagnostics. Micromachines 11, 1–7 (2020).
3. Peiris, J. S. M., Guan, Y. & Yuen, K. Y. Severe acute respiratory syndrome. Nat. Med. 10, S88–S97 (2004).
Recent Posts
-
Advanced Materials for Unmanned Aerial Vehicle (UAV) Protection Against Laser
Consider a UAV on a critical mission, rendered inoperative by a sudden laser attack. With the increa …26th Jul 2024 -
Simulation and Modeling of Material Properties
Our world is composed of a dazzling array of materials, each with its own unique properties that dic …19th Jul 2024 -
Advanced Coatings for Superior Corrosion and Wear Resistance
Corrosion and wear pose significant challenges across various industries, leading to substantial eco …12th Jul 2024








